Working at the limit
Working at the limit
There is perhaps no greater safety net in society than the local GP practice – but what happens when the intense working pressures mean it no longer feels safe to its staff? In the first of a series of articles ahead of the Welsh elections on 7 May, Seren Boyd visits a practice in a deprived part of south Wales, to hear doctors' priorities for the new government
Tricia Jenkins always said her last job would be in Marks & Spencer’s food hall, ‘watching everyone’s food go by’.
There’s a big store in the retail park on the north-west edge of Merthyr Tydfil, a short walk to the old Cyfarthfa ironworks and the town’s industrial past.
Yet, 37 years after joining the team at Pontcae Medical Practice, Mrs Jenkins is still there. She is now reception manager and she won’t leave – although the job has changed, along with the south Wales valley town they care for.
‘It is harder now, more pressure,’ she says. ‘All these patients wanting appointments and we’ve only so many doctors. But we’re such a good team here. If we say: “Trouble at the desk,” the practice manager or any of the doctors will come out in a minute.’
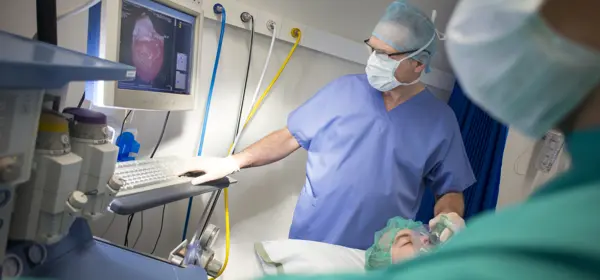
Just last week, Kevin Thomas, lead GP partner (pictured above, left), was summoned to pacify an angry patient demanding to be seen that day.
‘People just don’t realise what it is like behind the scenes and how busy everybody is,’ says Mrs Jenkins. ‘Then you get a thank you card from someone appreciating how much the surgery has done for them ... It’s still rewarding.’
Overwhelming demand
At the hub of this single-storey surgery screened by high hedges, practice manager Kevin Rogers is watching his plan for the day starting to unravel.
GP Kate Williams and others on the team are monitoring a patient for whom they have had to call an ambulance.
The patient receives all the time and attention they need – but, really, there’s no flex in a schedule where demand overwhelms capacity every day.
Mr Rogers has been in post here for 24 years and it has always been his job to balance competing pressures: acute and chronic, pre-bookable and urgent, premises and pay. But it has never been quite like this.
‘Every day now is a conundrum,’ he says. ‘We've planned the day to the best of our ability, and then you just have to see how things pan out. You just don't know what you're going to get.’
You're often having to manage things you don't feel you have the expertise for
Kate Williams
And it’s the same across this health board in South Wales. He chairs the practice managers’ group for Cwm Taf Morgannwg, and his colleagues paint the same picture. Five practices in the board area closed between August 2021 and October 2025. New patients register with Pontcae almost daily.
‘All the practice managers I speak to say: “This is really tough now,”’ says Mr Rogers, ‘but there’s no lack of desire to want to do a good job.’
The strong sense of team and a ‘really supportive environment’ is what motivates Dr Williams and colleagues to press on despite the pressure, they agree. They’re taking a short tea break together, signing prescriptions between sips.
Gemma Wheeler, who trained in Cardiff, feels ‘very lucky’ to be one of the ten GPs at Pontcae. GP posts have been harder to find since the new general medical services contract for Wales in 2023: Dr Wheeler applied for about 25 jobs before taking up a salaried post here last year.
‘It was so demoralising: I had a complete crisis of career,’ she says. ‘I felt like: I've trained in Wales, I know the local population, passed all my exams, and now no-one wants to employ me. I started applying for jobs in cafes. It was not a good time.’
Yet, primary care is not for the faint-hearted, not in Merthyr Tydfil nor anywhere in Wales, as BMA Cymru’s Save Our Surgeries campaign has made clear.
Merthyr still has high levels of deprivation, an ageing population and, according to the Office for National Statistics, the lowest life expectancy at birth for males in Wales (75 years). It has the lowest female healthy life expectancy (50.1 years) in the UK. A history of coal mining and heavy industry has left its mark. But its issues are not unique to Merthyr.
High levels of comorbidity among Pontcae patients and tight time constraints mean it is often hard for the team to feel they’re doing a good job.
Long specialty waiting lists too mean that more patients are now paying to go private for diagnosis. ‘Even though they don’t really have the funds,’ adds Dr Williams. Those who can’t pay keep coming back to Pontcae, increasingly frustrated, increasingly unwell.
‘You’re often having to manage things you don’t feel you have the expertise for,’ says Dr Williams. ‘We’re dealing with a huge breadth of stuff and everything’s interlinked, especially where patients are very comorbid. Trying to run to time and actually make a difference for someone can be very difficult.’
The heavy burden of acute need, especially since COVID, has locked the team in fire-fighting mode but they are making a concerted effort now to manage chronic disease more effectively. ‘But it’s quite difficult to find the time to fit it in with everything else,’ says GP partner Kate Marsh (pictured in main image, right).
As Mr Rogers points out, for diabetes alone, the National Institute for Health and Care Excellence-recommended ‘eight care processes’ involve a GP, physician associate, diabetic nurse and healthcare support worker.
‘We get 130-odd pounds per patient per year [for everything],’ he says, ‘so we’re expected to provide a full year’s general medical services for less than it costs for one consultation for my dog at the vet’s opposite.’
Eighty-two-year-old Laura Guard has come in to see Dr Thomas on her way to the gym.
A former biomedical scientist in the NHS, she has lived locally all her life, been a Pontcae patient for 27 years and used to chair the surgery’s patient participation group.
She does not mince her words: ‘I despair when people are not prepared to take ownership of their own health. A slight ache and they're running to the doctor. It’s a two-way thing: you’ve got to do your bit as well. This practice has got my full support: they’ve got a very difficult job.’
I felt like: I've trained in Wales, I know the local population, passed all my exams, and now no-one wants to employ me
Gemma Wheeler
Over-dependence on general practice is something the GPs worry about too. Whatever is fuelling it – health anxiety, lack of basic medical knowledge or (in some) a sense of entitlement – it has definitely grown since COVID, they feel.
If a child falls unwell at school, it is not uncommon for a parent to phone for an appointment even before they have collected their child and assessed the situation themselves.
A GP partner now sits with the care navigators, to help triage and signpost, as requests for acute appointments generally exceed what is available.
All this points to a wider problem that general practice is facing. It has become the destination for all unmet need as other services in society rein in their remits. As Mr Rogers puts it, ‘people assume everything is primary care’.
There are some positive spin-offs. For ten years, Pontcae and other local surgeries had ‘GP support officers’ – funded by the primary care cluster, managed by the health board – providing patients help with everything from housing to benefits. Since the health board withdrew its support last year, Pontcae has started collaborating with Citizens Advice to set up a similar project.
But, for Dr Thomas, it can feel as if GPs’ doors are being wedged ever wider through an ‘unlimited, open-ended’ contract, to the detriment of patient care.
‘We’re the safety net but it’s an unsafe safety net because we can’t do it all,’ he says.
Part of Dr Thomas’s time this morning has been spent providing extra checks and support for a number of patients on specialty waiting lists, at the behest of NHS Wales. As with the 100 or so other patients whom the practice has referred in the last six months, he has assessed that they should almost all remain on the list.
He says the government’s recent instruction to health boards to aim to reject at least 20 per cent of GP referrals is ‘absolutely appalling’.
‘Disrespect’ is a word that comes up often as he discusses how he feels general practice is being treated by politicians and health bosses.
‘Things are done to us, despite us and against our advice,’ he says.
‘We’re pitched between Welsh government and the public and we get battered by both sides, with government not discouraging the public to batter us. We’re just a political football.’
He is also tired of feeling overmanaged by a system which focuses on ‘process, not outcomes’, measuring the quantifiable rather than protecting patient care. Too much of his time as lead GP – at least a day a week – is spent on reporting and assurance, he says. ‘So much effort is put into making sure that we’re doing what we say we’re doing.’
General practice is front and centre of BMA Cymru Wales’ Senedd 2026 manifesto, Health in our hands. Specific asks include: establishing a national safe standard for working; restoring the proportion of the NHS Wales budget spent in general practice to 8.7 per cent within three years; reviewing the current GP funding model; investing in the GP workforce; and improving GP estates.
On Dr Thomas’s personal wish list for the new government in May, ‘resource’ inevitably features prominently.
‘Money underpins it all but this is not about pay rises,’ he says. ‘It’s about making sure practices survive.
‘Every time a government initiative comes along, like increasing employers’ NI, we get clouted. Funding has been purposefully eroded. Year on year, there’s less left after we pay the bills,' says Dr Thomas.
We’re just so fed up of being treated the way we are. Why is everything adversarial? There’s no trust whatsoever
Kevin Thomas
Primary care cluster funding, though recurrent, is set on an annual cycle in Wales. So long-term financial planning – on issues such as employing staff for cluster initiatives, like those GP support officers – is nigh on impossible.
Yet, for Dr Thomas, other priorities come higher up the list.
He wants GPs to have greater autonomy to attend to their own priorities: he’s inspired by the transformation that the Finnish education system underwent when the profession was allowed to make its own decisions. ‘If they just gave us free rein to do our best for patients, the outcomes would be much better.’ He adds, wistfully: ‘Fundholding was absolutely excellent.’
What he wants above all else, though, is respect for his profession.
‘We’re just so fed up of being treated the way we are. Why is everything adversarial? There’s no trust whatsoever.’
Fundamentally, his focus is better patient care: it is also his motivation for pressing on. Despite everything, as a ‘local boy’, he is deeply committed to the area, to the practice and to the job of a GP which he still finds ‘absolutely fascinating’.
‘When you get receptive patients, and the majority are, for whom respect works both ways, you can fix things for them. So, stick with this? Yeah, will do.’
- In March, a cross-party report by the Senedd’s health and social care committee on the future of general practice made a series of recommendations in line with BMA Wales’s Save Our Surgeries campaign, including significantly increased investment in general practice