In all honesty
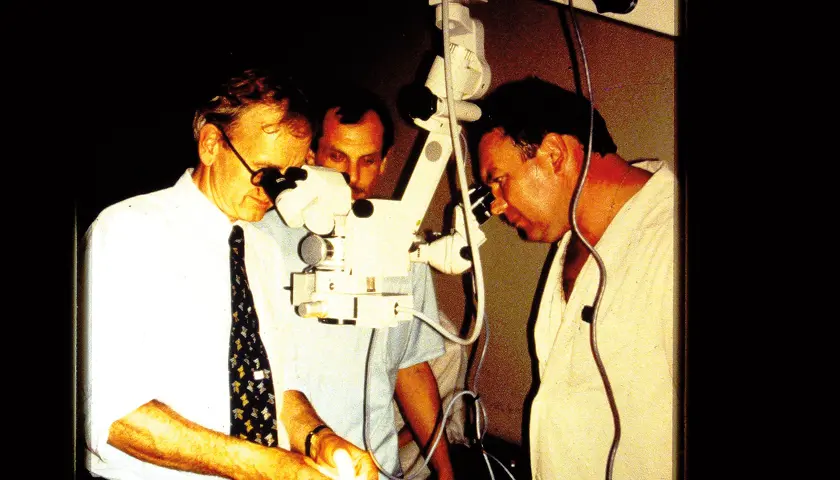
Henry Marsh has a reputation for frankness – with patients, colleagues, and about his own shortcomings as a neurosurgeon. Now he is a patient with a serious illness, he has become more honest with himself
Henry Marsh has just had a five-mile run and is in the thick of wall papering. Even before he retired from neurosurgery, he had always enjoyed DIY.
He is, in his own words, leading a normal life, but for the hormone therapy. Two years ago, he was diagnosed with advanced prostate cancer and his life expectancy dwindled to a few years.
Today, after treatment, he’s in remission. In the interim, he’s wrestled ‘with philosophical and scientific questions that suddenly seem very important’ and come to terms with the idea of dying.
‘At 72, the future’s uncertain anyway,’ he says cheerily. These are some of the themes explored in his new book, And finally: matters of life and death. Last month, on a visit to Ukraine, where he’s worked for 30 years, he had to tell a young man that his brain tumour would be fatal.
It is a thankless task he has had to perform endlessly in a nation where the most desperate cases find their way to his clinic. This time, however, it was different.
‘I could talk to him man to man about what it’s like to have an uncertain life expectancy,’ he says, ‘although at my age it’s profoundly different from being in your early 30s. Being a patient is frightening and humiliating and demeaning… and I think doctors often underestimate, and don’t really understand, what it’s like.’
His self-deprecating memoir, And finally, recounts his abrupt fall in the hospital hierarchy from eminent brain surgeon to patient ‘Marsh: five, three, nineteen-fifty’.
Among the London hospitals he attended as a patient was one he used to visit weekly for conferences with neuro-oncological colleagues about brain tumour cases.
‘I could feel myself lose height as I walked along the corridor,’ he writes. But he embraces the indignity of it all, discussing urine flow and rectal clinics with brutal honesty and wry humour.
He’s furious with himself for the self-denial that made him put off seeking advice about prostatic symptoms.
Dr Marsh, senior consultant neurosurgeon at St George’s Hospital in London till 2015, has retired from clinical work in the UK. He suspects his experiences of the last two years would make it ‘very difficult’ for him to do the job now.
In his words, he’s lost the capacity for ‘self-deception’, the necessary confidence to wave aside self-doubt and disengage emotionally in the face of complex medical challenges. Empathy, an unexpected side effect of his close encounter with death, has undermined all that.
Much to my surprise, I now feel a more complete human being
Dr Marsh
He describes sorting through old case notes during lockdown – and being ambushed by memories and emotion.
‘It’s only when doctors become old enough to become patients themselves or their family become patients that you get a sort of insight into just how detached we become as doctors,’ he says.
‘We have to be detached: we couldn’t do the work if we didn’t. ‘I think I could have been more sympathetic with patients than I was, but I don’t know if that would have made operating more difficult.
‘I was incredibly lucky to have had the career I had and the NHS at its best, which was probably 15 years ago or so. But I don’t miss it: I’m relieved not to. Much to my surprise, I now feel a more complete human being. I no longer feel split down the middle, having to divide humans into us and them, patients and the medical profession.’
Working in Ukraine
In Ukraine, by contrast, Dr Marsh’s work is not over – and it’s been profoundly upsetting for him to watch the conflict unfold since February.
In March, he worked with renowned war surgeon David Nott to deliver online surgical training to hundreds of healthcare professionals in Ukraine.
But he’s at pains to point out that Ukrainian clinicians are experienced in battlefield medicine: the current conflict began with the Russian annexation of Crimea in 2014.
He remains in regular contact with his many friends and colleagues in Ukraine. As recently as August, he visited Lviv, ‘saw a few patients to help a colleague out’, and met with the minister of health.
‘I sat in my favourite café in the old market square in Lviv and it’s unchanged,’ he says. ‘Very strange. There are the occasional air-raid sirens and they are very distressing, but the chances of being hit by random missile strikes there are fairly small.’
As And finally recounts with blistering frankness, his working relationship with Ukraine has changed since his 20-year collaboration with a colleague ended abruptly.
He devotes his time to supporting younger surgeons whom he describes as unhindered by Soviet-era thinking. And he has good relationships now with the senior professors who used to regard him as ‘the devil incarnate’ for his pioneering work there.
The need for honesty
One reason he gives for the breakdown in relationship with his Ukrainian former colleague was a lack of honesty about his success rates.
Post-surgery complications, even deaths, were being hidden from him. It’s been a painful time which has caused him to reassess his legacy in Ukraine – but also reinforced the importance of honesty, a ‘compulsion’ and recurring theme of his.
Dr Marsh has, for example, been an outspoken advocate of assisted dying and writes bluntly about having a ‘suicide kit – a few drugs legally obtained’. He’s no longer afraid of death, but he won’t countenance dying with dementia, his father’s fate.
I went into the profession keen, ambitious, individualist, egocentric and egotistic
Dr Marsh
He’s also written and spoken extensively about the need to be honest with patients about their prospects, and having the courage not to operate when surgery won’t help. The heart-rending repercussions of this for the many Ukrainian patients he sees with inoperable tumours are played out in the BBC’s 2007 documentary about him, The English Surgeon.
Living with failure – whether unsuccessful surgery or declining to treat – is ‘what makes medicine special’, he writes. His openness about his own mistakes is partly what has made him famous.
He fears that the culture of litigation and criticism means it is sometimes difficult for doctors to be fully honest with patients, colleagues, even themselves. ‘The real test of a doctor is when things don’t go well,’ he says. ‘There’s nothing special about success.
I think it’s terribly important we are honest and realistic about what the work is really like, although there’s nothing more frightening for a patient than a frightened doctor.
That’s a very difficult balance we have to strike. ‘Medicine is all about feelings, communication, dealing with colleagues and patients, decision-making and all that leads up to an operation. That’s the difficult bit. The actual technical operating side of surgery is, in one sense, easy.’
Team working
Dr Marsh may no longer work in the NHS as a clinician but he is still passionate and outspoken about it. He insists that doctors need supportive colleagues and a collaborative culture if they are to learn to sit with failure and not be damaged by it.
‘I went into the profession keen, ambitious, individualist, egocentric, egotistic, as I think most surgeons are, and I’m leaving it a passionate believer in team working,’ he says.
‘If you’ve really good colleagues, your decision-making will be better. And it is vital for your mental health. ‘The generation who trained me were like lonely gods and I think, in neurosurgery, many of them were a bit damaged as a result. Real teamwork means discussing difficult cases. Multidisciplinary team meetings are a step in the right direction. But the art of conducting a good clinical meeting is incredibly important and it is not really taught at all. It is vital to a happy, successful department.’
The generation who trained me were like lonely gods
Dr Marsh
He worries especially for junior doctors who don’t feel they have the support of their seniors. He cites psychiatrist Simon Wessely’s finding that one of the factors that makes post-traumatic stress disorder in soldiers more likely is poor leadership.
‘In a big general teaching hospital, it is very difficult to create that sort of “family firm” atmosphere which my generation had, and which helped you cope with what is a deeply stressful job.
‘We need good leadership in consultants. They are the longest-serving people in hospitals but consultants have in a sense been emasculated in the NHS. Chief executives come and go and make no impact.’
‘Pathetic, crying’
The past two years have been tough, as he has observed his own physical decline, and his ‘lifelong obsession with death and suffering’ has become personal. He has been rocked before, when his son William was treated (successfully) for a brain tumour as a baby – and his wife, anthropologist Kate Fox, suffers from Crohn’s disease.
But he admits he was completely thrown when his initial ‘sky-high’ PSA (prostate specific antigen) of 127 suggested that he had metastatic disease.
‘I was panic-struck, pathetic, crying, everything else,’ he says. ‘But also I felt very strongly I’d had a fantastic life. I need to live longer for my wife, for my children, my family. But for myself, I’ve had my cake and eaten it. I’m pretty privileged and lucky: in my parents, my upbringing, my education, my experiences. I’ve been quite successful. And I’ve no bucket list whatsoever.’
His cancer proved only locally invasive. After radiotherapy and hormone treatment his PSA is now low – an update given in postscript – although his original PSA puts him at high risk of recurrence within five years.
For much of the book, however, he’s staring death in the face. In the final paragraph, he considers what physicists call ‘block time’, where past, present and future are equally real, as if his life is flashing before him.
Surrounded by mysteries
For now, he’s well and determinedly optimistic. He believes, for example, the NHS is ‘perfectly solvable with a different government, properly looked at, properly funded’.
He’s increasingly speaking out on climate change too and his belief that we each have a duty to try to reduce our carbon footprint. More DIY home improvements, maybe new plumbing to enable grey-water harvesting, will undoubtedly follow – although his book suggests strongly he’s a better brain surgeon than builder.
He even plans to write a children’s book about Olesya, the hero of the stories he told his granddaughters over video calls for two years during COVID. His long fascination with philosophy – a subject he studied, and dropped, in his first degree at Oxford – has resurfaced too.
If only more people were better at saying, “I don’t know but let’s try to find out
Dr Marsh
And finally is full of ellipses, as forays into scientific explanation are mingled with moments of star-gazing, where the metaphysical defies human intellect and understanding.
As in his first book, Do no harm, he’s still exercised by the question of consciousness – whether it arises from physical processes or ‘something we cannot know’.
But he can accommodate mystery and unanswered questions these days. Almost.
‘I love the not knowing,’ he says. ‘The really important things I don’t know. If only more people were better at saying, “I don’t know but let’s try to find out.”
‘We are surrounded by mysteries and that’s wonderful. It’s like opening a door and facing a room with a lot more doors.’
- Until September 2024, resident doctors were referred to as ‘junior doctors’ by the BMA. Articles written prior to this date reflect the terminology then in use