Doctors raise alarm on ‘unsafe and distressing’ substitution
Doctors raise alarm on ‘unsafe and distressing’ substitution
As the BMA publishes a survey of 5,000 doctors on the role of advanced practitioners, Ben Ireland takes an in-depth look at how widespread they say this scope creep has become
‘Where I work, advanced practitioners (APs) are essentially doing the same job as doctors’.
A specialist, associate specialist and specialty (SAS) doctor responding to a BMA survey on doctor substitution spells out the increasing concern among many of their medical colleagues.
They continue: ‘Many APs are working at the level of senior registrars, and lead APs are working at what is described as “consultant level”. Management even appoints APs as clinical supervisors for doctors.
‘Patients often assume these APs are doctors. When concerns are raised, management dismisses them and insists that APs are properly trained and working at the level of senior doctors.
‘In reality, APs are taking jobs that would normally be done by doctors. They cover doctors’ annual leave and sick leave and carry out almost all clinical duties expected of doctors. The only thing they do not do is write death certificates.
‘In my view, doctors are still employed mainly so that responsibility and blame fall on them when something goes wrong. Overall, this is a very unsafe and distressing situation.’
The results of the BMA survey of more than 5,000 members back up the worrying picture this doctor paints, of how often APs are being deployed beyond their scope by employers filling gaps in doctor rotas, being asked to diagnose patients, prescribe medication and make independent treatment decisions which they are not qualified for.
Not doctors
APs were first introduced to the NHS in the late 1980s and early 1990s, a time, like now, of doctor shortages. The role was designed to offer expertise in a specific field – but strictly within the scope of the base profession, be it nursing, physiotherapy, occupational therapy or pharmacy.
NHS England describes APs as ‘accomplished registered health and care professionals’ working at ‘a level of practice characterised by a high degree of autonomy and designated responsibility for complex decision making’, underpinned by master’s level qualifications.
But they are not doctors.
The NMC (Nursing and Midwifery Council) confirmed last month that ‘advanced practitioners are not a substitute for medical practitioners’, and while the RCN (Royal College of Nursing) says APs are ‘highly-skilled experts in their own right’ it accepts they are ‘not replacements for doctors’.
The RCOT (Royal College of Occupational Therapists) says APs are ‘regulated professionals working within defined scopes of practice’ and ‘are not substitutes for other professions’, adding: ‘Advanced practice is not the problem. The issue is how these roles are defined and used across the system.’
Yet freedom of information requests by the BMA found that almost half of trusts are employing APs in doctor roles, in what it dubbed a ‘haphazard approach’ by NHS management.
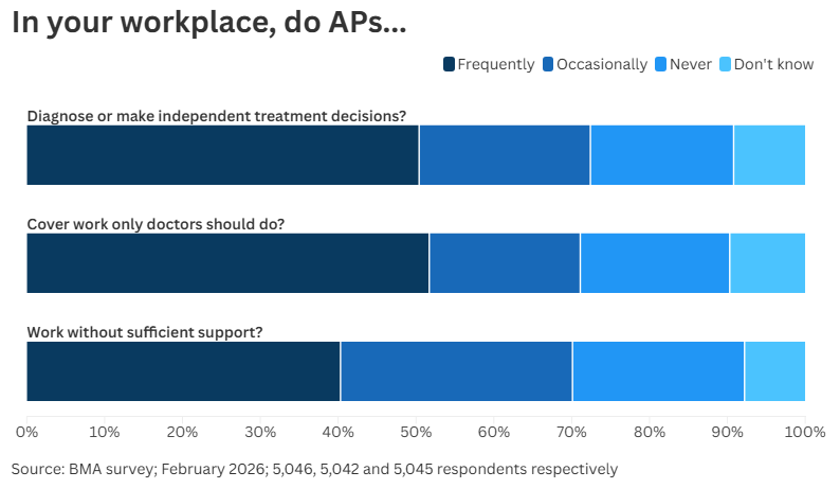
Three quarters of doctors and medical students who responded to the BMA survey said they are concerned about APs working beyond their competence and 72 per cent said APs in their workplace diagnose and make independent treatment decisions that should only be made by a doctor.
Seven in ten respondents said they have seen APs cover work that should only be done by doctors and a similar number have witnessed APs working without sufficient support from senior doctors, such as consultants, GPs or SAS doctors.
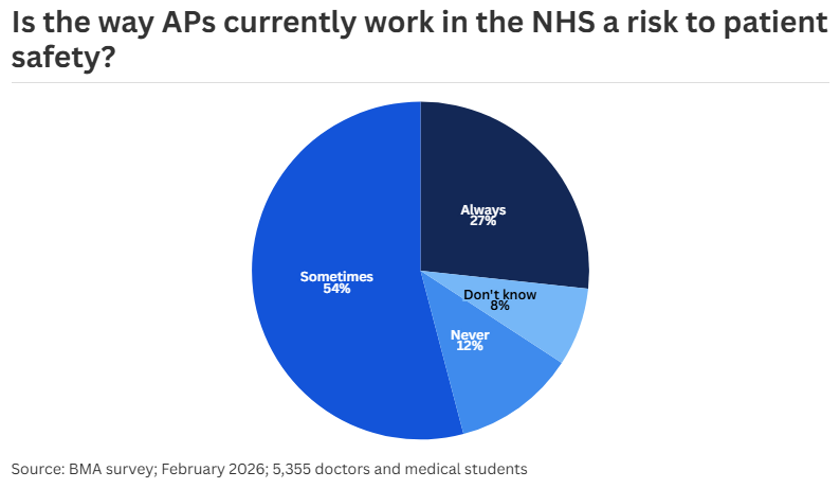
Four in five respondents to the BMA survey said the way APs currently work in the NHS is a risk to patient safety.
Tragic consequences
The consequences of this scope creep can be, and have been, tragic.
Rotherham NHS Foundation Trust apologised last year after 68 patients either died or suffered complications within 30 days of a procedure at an endoscopic retrograde cholangio-pancreatography (ERCP) service led by a nurse consultant.
A review by the Royal College of Physicians found failures in the care of 58 patients, while 25 ‘suffered some degree of harm’. The college noted the ‘unusual circumstances of a nurse providing interventionist procedures’ and recommended ‘the ERCP service should move to a medically qualified, consultant-led service’.
The widower of Valerie Birkill, who died three weeks after her procedure, told the BBC he will ‘never forgive’ Rotherham Hospital for the poor care she received.
The 73-year-old had suffered a perforated bowel, but when her family raised concerns after the treatment they were told she ‘probably had trapped wind’.
After the RCP review, her husband Garry said: ‘Our family will never be the same without Val. We knew we owed it to her to get answers regarding her care but it was still devastating when the trust admitted Val would have made a full recovery if she had received the correct care.’
'De facto SHOs'
Doctors’ responses to the BMA survey show how frequently APs are being employed beyond their scope.
Examples given include APs working as ‘de facto SHOs’, working on-call shifts and holding bleeps, and acting as a ‘senior clinical decision maker’. One response said there was not a single doctor covering a neonatal centre staffed exclusively by ANNPs (advanced neonatal nurse practitioners).
A consultant said they had seen APs miss tumours on CT scans and incorrectly diagnose a patient with Crohn’s disease.
‘The attitude of the advanced practitioner is that everyone makes mistakes, so it is OK,’ this consultant added. ‘It would appear that consultant expertise is not valued and it does not matter if patients are harmed. There is no regulatory framework to protect patients.’
APs are taking jobs that would normally be done by doctors… the only thing they do not do is write death certificates.
SAS doctor responding to BMA survey
Melissa Ryan, a paediatrics ST4 in the East Midlands and a former co-chair of the BMA’s resident doctors committee, told The Doctor that the way APs are currently being deployed in the NHS ‘should be ringing alarm bells’.
‘You have people essentially working as doctors who do not have the training to do so and we are getting errors,’ she says. ‘Those errors can be made without realising, because they don’t know what they don’t know. It’s not safe.’
Dr Ryan is on the BMA’s steering group on doctor substitution and says there are parallels between the deployment of APs and that of PAs (physician assistants) and AAs (physician assistants in anaesthesia), roles investigated in the Leng Review – which concluded there was a ‘lack of clarity’ including ‘confusion with a doctor’.
The Leng Review recommended that PAs ‘should not see undifferentiated patients except within clearly defined national clinical protocols’. Yet the BMA says employers continue to flout Leng's recommendations, despite them being accepted in full by the health secretary.
Legislation going through parliament is expected to reduce confusion for patients by retitling PAs, but this would do nothing to clarify the role or title of APs.
About 80 per cent of survey respondents said APs are considered by employers as equivalent to doctors in their workplace, and some 90 per cent said APs should never be considered equivalent to doctors.
‘Trusts are running rotas where they count APs within medical staffing,’ says Dr Ryan. ‘Shifts [on medical rotas] get put out to APs. It’s rare to have departments that don’t have APs now if the trust or board employs them.’
The decision to do this is one for individual trusts, or boards in the devolved nations, which set the level of scope for APs at a local level.
‘Some of the decisions to use more APs come down to funding, and some come down to departmental pushback,’ explains Dr Ryan. ‘We know of some trusts culling locally employed doctor (LED) roles and replacing them with APs.’
About three quarters of doctors surveyed think the public do not understand the difference between APs and doctors.
‘You’ll often hear APs, and PAs, saying they are part of the medical team,’ says Dr Ryan. ‘They should be making it clear they are not a doctor. You can’t expect a patient to know the difference.
‘It matters because if something should happen, you’d want a patient to know they were able to ask a doctor for a second opinion. But if they don’t know who has seen them then they might not know to escalate that.’
Dr Ryan says the public are more likely to understand the difference between a nurse and a doctor, or a physio and a doctor but can be confused by the term ‘advanced practitioner’, perhaps assuming they are a type of doctor.
To make the distinction clearer, she would like to see the roles changed to emphasise the base profession of an AP, to make it explicit that they do not have medical training and should not be used to substitute doctors.
One suggestion is the introduction of national scopes of practice, with limits, for APs.
The survey results come amid a wider rollout of APs in the NHS. The government’s 10 Year Health Plan for England says it intends to ‘develop advanced practice models for nurses and other professionals’ and ‘increase the number of nurse consultants’.
NHS England chief executive Sir Jim Mackey was quoted by the Health Service Journal during recent strike action as saying the NHS will ‘reduce our reliance’ on resident doctors, which Dr Ryan says is ‘saying the quiet bit out loud’.
You have people essentially working as doctors who do not have the training
Dr Melissa Ryan
Doctors are not against the role of APs in principle. Some consultants responding to the BMA survey said that APs undertaking tasks within a safe scope can be helpful to the running of their services.
And as the Nuffield Trust pointed out back in 2016, ‘a shortage of junior (now resident) doctors is driving a significant growth in advanced practice roles’.
The point stressed by the BMA is to ensure that the limitations of APs’ scope is understood, adhered to and regulated effectively. ‘For this to happen, we need to ensure there is no local variation and blurring with doctor roles,’ says Dr Ryan.
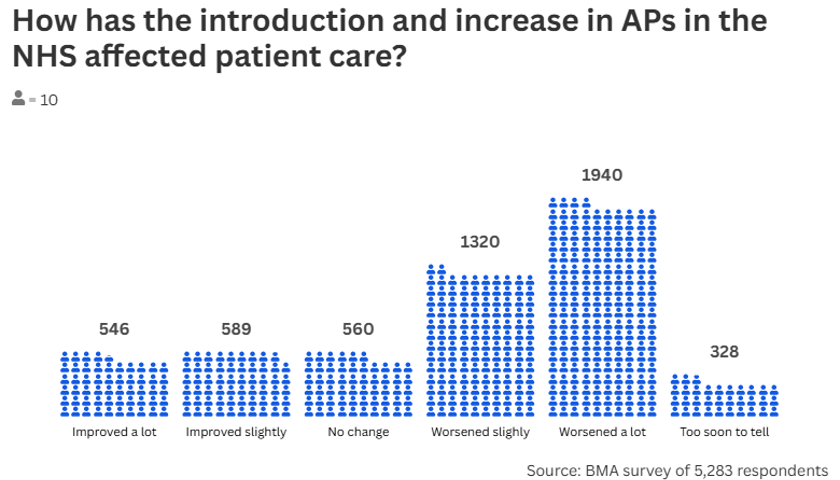
A majority of doctors responding to the BMA survey believe the introduction and increase of APs in the NHS has worsened patient care.
Dr Ryan explains that APs, without the depth and breadth of medical training, are not fully equipped to deal with complications, or may not even notice them in some instances.
She says: ‘If something goes wrong in a procedure, you need to be able to know how to deal with that very quickly or the patient will get very unwell.’
The government’s move towards ‘taskifying’ healthcare has gradually developed but picked up pace in recent years, says Dr Ryan. She says current deployment in the NHS has now gone beyond the first principles of the AP role, which was intended to be supervised by a doctor who would remain responsible for diagnosing a patient, set the treatment plan and be on hand to deal with any complications.
‘Enhanced practice, in principle, is fine,’ she says. ‘We need more people on the ground, but what we don’t need is people without enough knowledge and training being asked by employers to do roles where there is risk to patients.’
‘But over time the amount of professional experience needed to become an AP has reduced.
‘Universities are no longer just taking a very experienced nurse, for example, with 5-10 years of experience. They’re also taking staff with as little as two years’ work experience.
‘Some universities do not specify any minimum experience requirement at all, so potentially a recent graduate could apply, negating the myth that these are highly experienced individuals upskilling their clinical acumen.
‘In addition, trusts have broadened where these staff are used – often in places where we’ve got doctor gaps. They can go from being a physio one day with all of the limitations around the role, to being a trainee AP the next and suddenly allowed to see undifferentiated patients, often with little supervision.’
Dr Ryan says emergency care, general practice and paediatrics are hotspots for APs undertaking tasks that should only be done by a doctor, because for years there have not been enough specialty training places for resident doctors to meet increasing patient demand in those disciplines.
APs are also permanent members of staff at a trust, unlike resident doctors in training who rotate between trusts to gain experience. This can be to the detriment to those doctors’ training opportunities, says Dr Ryan.
‘Resident doctors are just not getting the training,’ she explains. ‘Trusts are prioritising APs who are likely to stay in the department instead of resident doctors who are going to leave in 4-6 months.
‘In A&E, resident doctors – who can be relied upon to differentiate patients – tell me they are pushed towards the minor stuff, churning through patients in A&E, but don’t get to do any of the work in resus. Instead, the consultant takes the AP with them because they can confidently rely on the doctors to manage everything else.’
She adds: ‘It makes it very difficult for doctors in training to learn the skills they need to become a consultant, and they worry that the future consultant workforce will not be as skilled as a result.’
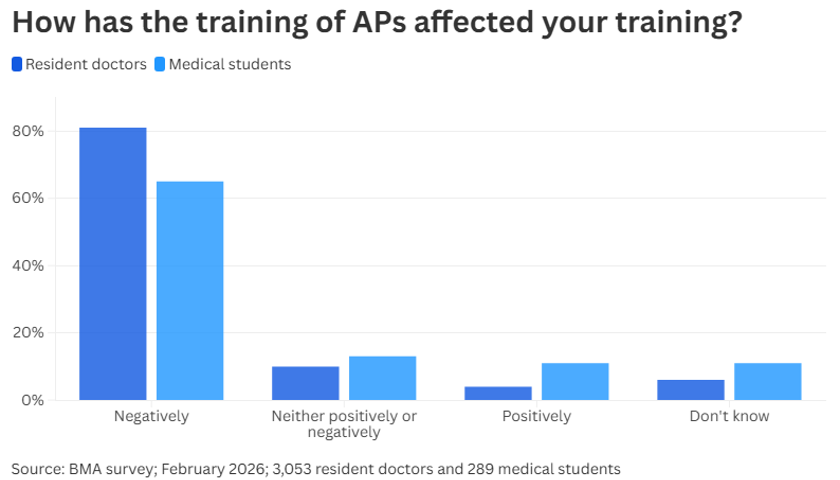
Survey data backed up the point, with both resident doctors and medical students reporting the training of APs having a negative impact on their own training.
Causing resentment
Dr Ryan says this approach to training creates a situation where APs get ‘all the good bits’ of being a doctor without the more difficult tasks, the discharge summaries, night shifts and on-calls, and ultimately the responsibility if something goes wrong. This, she says, is ‘causing resentment among a whole generation of resident doctors, who often have to mop up the errors they see while feeling unappreciated’.
AP nurses (ANPs) are regulated by the Nursing and Midwifery Council (NMC) for their nursing duties, but are not specifically regulated as advanced practitioners, as pointed out by the Nuffield Trust in 2023. ‘It makes it really difficult to officially determine whether something is safe or not because the regulator doesn’t have full oversight of current advanced practice,’ says Dr Ryan.
With as little as two years of advanced practice training (on top of the base nursing qualification), employing APs can be attractive to employers looking to fill gaps amid a shortage of doctors, and with doctors leaving the country for better pay and conditions overseas.
‘Some consultants would say that their service would fall over without APs,’ says Dr Ryan. ‘But that doesn’t make it safe.
‘APs may be cheaper than some senior doctors and trained more quickly. But faster training doesn’t lead to a quality service if the role involves working beyond safe parameters and without adequate oversight.
‘In an absence of doctors, we need something, otherwise we would have to close the service. But when APs were first introduced, I don’t think doctors realised how far this would go.
‘We do not have a problem with advanced practice per se, there is absolutely space and a need for well-defined safe roles. We have patient demand there. But what we don’t need is the blurring of boundaries with the role of a doctor and unsafe practice.’
‘Specialists in their fields’
The RCN’s chief nursing officer, Lynn Woolsey, says nurses working at an advanced level are ‘assessing, planning and co-ordinating the delivery of care as specialists in their fields’ and that ‘without them, the health service would grind to a halt’.
She says ‘patient safety is non-negotiable for both doctors and nurses’ and called for employers to ‘ensure all services are staffed with the right number and mix of clinical professionals’.
But she warned the BMA that ‘waging professional warfare through staged media interventions rather than working in collaboration risks eroding professional cooperation and public trust’.
‘We appreciate that doctors want investment, but their campaign will not be helped by undermining an entire advanced level of nursing which is in fact safe, effective and valued by patients,’ she says.
The CSP (Chartered Society of Physiotherapy) said the BMA survey of doctors was 'self-selected' and that APs 'have an exceptionally strong record on safety'.
Chief executive John Cowman said: ‘The NHS needs more doctors to ensure rotas can be appropriately staffed and patient needs met.
‘However, that point stands alone. We should be wary of making any assumptions that rostering or rotas reflect the quality of care patients receive from AHPs or nurses working at an advanced level.'
Caroline Waterfield, director of workforce supply and employment practice at NHS Employers, says: ‘High-quality patient care relies on teamwork and the need to be able to draw on the expertise and skills of a number of different health and care professionals at the right time.’
She said employers have protocols stipulating that all staff ‘practise in compliance with their respective code of professional conduct, within their scope of practice and ask for help when needed’. The NHS England Centre for Advancing Practice, she added, has published advice, guidance and governance tools for employers ‘to support the effective implementation of advanced practice in clinical settings’.
‘When introduced with clear purpose and proper support, advanced practice roles can help employers redesign services, strengthen multidisciplinary working and leadership, expand workforce capacity and flexibility, improve the continuity and quality of care for patients and enhance staff experience,’ says Ms Waterfield. ‘These benefits can be realised when advanced practice is planned as part of a wider workforce approach with clear role design and governance. It isn't a short‑term fix for immediate pressures.’
Tom Dolphin, a consultant anaesthetist and chair of BMA council, told The Doctor: ‘The BMA has been saying for some time that doctor replacement is not good for patients.
‘Some managers and politicians believe doctors can be replaced by other healthcare workers who have been “trained to task”, but medicine can’t be endlessly subdivided into tasks like that.
‘At various points you need to apply medical judgement, otherwise the overall picture is lost and things start to go wrong, as we’ve seen in too many tragic cases already.
‘People are forgetting the value of our long, rigorous medical training, and the irreplaceable breadth and depth of knowledge it brings. APs have a valuable role to play in some services, but the role is not that of a doctor.’