Humanitarian line, westbound
Humanitarian line, westbound
As Ukraine faces another Christmas fighting for its survival, a remarkable medical team transports the sick and wounded on a specially adapted train. One of the doctors tells Seren Boyd about life on board.
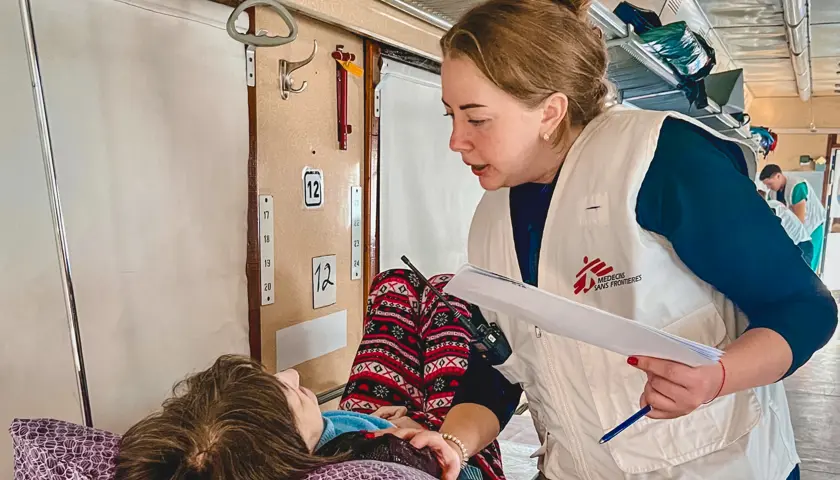
As the train bucks and sways, Nataliia Pivovar holds the teenager’s gaze and his hands, speaking to him gently. He plays with the rings on her finger.
The 17-year-old evacuee from Kherson has cerebral palsy: he can’t talk and is visually impaired. A few hours ago, the hospital he was in came under shelling by Russian forces. Now he’s on the medivac train run by MSF (Médecins Sans Frontières – also known as Doctors Without Borders).
Playing with the rings on Dr Pivovar’s finger seems to ease his distress and bring him peace.
Dr Pivovar too finds comfort in those rings, especially on the medical train. Before her MSF colleagues could start the evacuation from the hospital in Kherson, they had to take refuge in a bunker amid the shelling.
‘When I need to relax or calm down, I roll the rings around my finger,’ she says. ‘It’s such a small thing, but it connects me to home and gives me a sense of peace. It gives me strength.’
Dr Pivovar will often pause between carriages, to take a moment and twist her rings. She’s made more than 100 trips on the medical train, but she still finds it hard to forget the look in patients’ eyes.
Triumph of planning
The MSF medical train has been running since March 2022, soon after Russia’s full-scale invasion of Ukraine, transporting thousands of
sick and wounded civilians from areas close to the front line to safer areas in central and west Ukraine.
In a joint project between MSF and Ukrainian Railways, carriages from the 1980s have been heavily modified to create a novel addition to Ukraine’s health service in a time of war.
The patients being transported may be war-wounded or injured, have chronic diseases, psychiatric disorders or disabilities. Almost all of them need specialist medical care.
The front line is very close and we can hear explosions.
Dr Pivovar
The medical train, which MSF describes as ‘a cross between an ambulance and a state-of-the-art intensive care unit’, is a triumph of careful planning and resourcefulness.
Its intensive care unit is connected to the generator near the engine by 2km of electrical cabling. Carriages can be added, removed or reconfigured depending on the number and type of patients being transported.
‘We have some equipment that is not even available in every hospital,’ says Dr Pivovar.
The train has been busy, notching up more than 130 journeys so far.
Backdrop of war
Meanwhile, Ukrainian forces continue inching forward in their counter-offensive: having resisted Russia’s assault on the north and the capital Kyiv, they’re now trying to break through Russian defences to the east and south.
Kherson, where this medivac is being made, is strategically important as the gateway to the Russian-held Crimean Peninsula and has suffered heavy Russian bombardment in recent months. Eighty per cent of all healthcare facilities in the region have been damaged or destroyed.
As the Russian military continues to target health facilities, with blatant disregard for international humanitarian law, the BMA has repeated its calls for the neutrality of healthcare services and professionals in Ukraine to be respected.
Place of safety
In today’s evacuation, from a hospital in Kherson, many of the patients have limited mobility; most are elderly, suffering with dementia, cerebral palsy or other neurological conditions.
Because of their conditions, it was very difficult to evacuate them to bunkers in time when their hospital was shelled. That’s why the Kherson regional health authorities called on MSF’s help, to relocate these patients to other hospitals.
Dr Pivovar describes the confusion as patients are brought on board.
‘The front line is very close and we can hear explosions. Some elderly people have impaired hearing so they aren’t sure what’s going on. They ask us if everything is alright. I have to reassure them, saying, “everything is calm. It’s important to get on the train now, and we’ll soon take you to a safe place”.’
Dr Pivovar works her way through the patients, checking blood pressures, giving medication. In carriages with upper and lower bunks, she makes a point of putting the psychiatric patients on the lower ones. ‘It’s important for patients with psychiatric conditions to feel the floor under their feet,’ she says. ‘It makes them feel calmer.’
The journey from Kherson to the far west of Ukraine takes 36 hours and there’s little time for Dr Pivovar and the team to rest. Once they’ve attended to immediate medical needs, they make tea and serve sandwiches, which helps calm the patients further.
Serving in conflict zones is stretching. Dr Pivovar is a paediatric anaesthetist, but postgraduate training in psychology has proved invaluable too. ‘You need energy, strength and calmness to find a suitable approach for each patient, answer all their questions and make them feel safe.’
An ICU that rocks
Dr Pivovar has got used to most things on the train – including inserting cannulae in an intensive care unit that rocks. But it’s a strangely intense working environment, working in a long, thin tube, with everything and everyone at close quarters.
At the end of the journey, the medical team gathers in the staff carriage to eat, chat and decompress. ‘We discuss things unrelated to work and cook something delicious,’ she says. ‘Later, after the trips, the team tries to get together and spend time in nature, go for a meal, or do other recreational activities to help us unwind.’
But it can be hard to disengage fully.
‘You remember almost everyone, what condition the patient had, what they had gone through and what their
hopes were.’
Most patients on the medical train, wherever in Ukraine they are evacuated from, come with little more than a small bag. Some may return to their towns and cities after treatment but many won’t: their homes no longer exist.
‘Some patients go to relatives, some go abroad, and for some our social workers try to help find dormitories and houses for them to live in.’
MSF also helps provide medicines and essentials such as hygiene kits, as well as support with replacing lost identity papers or finding work.
You need energy, strength and calmness to find a suitable approach for each patient.
Dr Pivovar
Dr Pivovar feels for them; she had to rescue her own grandmother from her Russian-occupied village. ‘People ask me if it will be safe at their new destination and if they will return. I think about my own grandmother and how difficult it is for the elderly to change their surroundings and living conditions.’
Dr Pivovar mentions a woman of about 60 years of age with pulmonary fibrosis who was on oxygen and whom MSF transported twice for tests and specialist care, along with her husband. She was eventually told she needed a lung transplant.
‘They told us that we had become their family because, at a time when their relatives refused to help, complete strangers helped them.
‘They were very grateful and hugged us goodbye.
‘After words like that, you understand that your work and your attitude are vital for patients, because nowadays people forget about humanity.’
‘No right to be sad’
Last year, Dr Pivovar spent Christmas Day at the hospital in Kharkiv, in north-east Ukraine, where she works in both the paediatric intensive care unit and the emergency department.
Knowing her country was at war last Christmas was no excuse for being anything less than cheerful on the wards.
‘You simply have no right to be sad during the holidays because, working with children, you first have to make a holiday for them,’ she says.
‘Children in intensive care without their parents are very sad. So, you want to give them attention, entertain them, make them smile and give them small gifts. Their smiles are the most fantastic gratitude for our work.’
Unlike the MSF train, where she’s worked since June 2022, her own hospital often runs short of medicines and medical supplies. She regularly ‘fills gaps’ from her own purse.
She’s never thought of leaving Ukraine herself, though she has tried to persuade family members to go abroad.
‘I wanted to take my mother and grandmother abroad, but they refused because this is their home,’ says Dr Pivovar.
‘I love my city, my country, and I understand that I am needed here, especially now.
‘I hope we will be able to celebrate Christmas this year. However, we cannot predict when and where our help will be needed: we’re always ready to work. Admittedly, war causes sadness and does not allow us to celebrate holidays as before, but people can adapt to anything and find happiness in small things.’
It’s almost two years since the full escalation of the war in Ukraine, and the media is frequently distracted now by other conflicts. But Dr Pivovar remains focused on her work and committed to her people: Ukraine is still home.
‘Ukraine is a strong country and what is happening here with the war deserves to be known. I do not believe that the world will forget about Ukraine.’
With additional reporting by MSF