Back from the brink
Back from the brink
How does a close encounter with death influence your attitude to life and work? Two doctors tell Seren Boyd how confronting their own mortality has shaped their views on life
‘Nine lives’
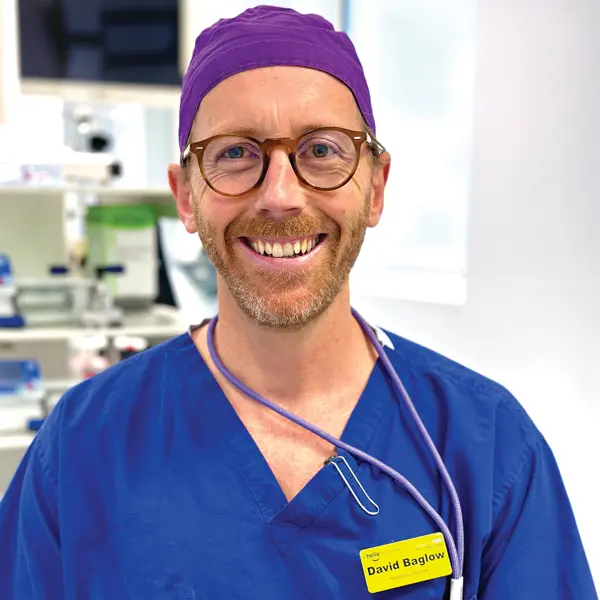
David Baglow’s mother tells him he has used his nine lives. He nearly drowned while surfing. A car slammed into him while he was cycling to work, causing serious injuries.
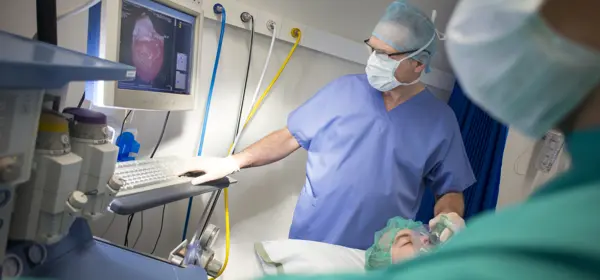
He suffered traumatic brain haemorrhages and then, eight months later, a stroke. And all this before he reached 41. Dr Baglow survived and was able to continue his anaesthetic specialist training.
He is now working in London and determined to make the most of life. He has a healthy respect for death and doesn’t take the risks he once did – but he’s not ‘fearful of the end’.
‘It’s the only certainty in life that everyone shares,’ he says. ‘I was annoyed, furious, at myself when I was underwater. I was thinking about my mum and sadness towards her after I was hit by that car and my vision was narrowing. And it was about three or four months after what happened to my head that I started to realise the gravity of it all.’
Of all his close shaves with death, it was the brain haemorrhages that were hardest to recover from, not least because they remain unexplained. Sussex police told him foul play was the most likely cause. He doesn’t remember anything of that evening in the pub with friends, or the week before.
Not drunk
He knows he wasn’t drinking much, which friends confirmed, as he was preparing for a big bike race. He disappeared during the evening and was found 11 hours later by police, collapsed outside the pub’s fire exit.
Assuming he was drunk, police took him home but within hours he had been admitted to ICU. His recovery took 18 months.
‘In hospital, I remember trying to walk and feeling like I was on a ship on stormy water. And I remember a horrific shuddering pain in my head from sound, lights, movement, seeing NHS written all over me, and nothing making sense.’
When he later returned to the same hospital as a trainee anaesthetist, some consultants would react to him standing in front of them with tears in their eyes. He appreciates how ‘hugely lucky’ he is. ‘And I’ve accepted that survivor guilt will subconsciously never leave me.’
'We don’t often discuss quality of life, which is much more important than the time you have left'
Dr Baglow
Yet, it was something that happened in his teens that had the most profound effect. Two days after a New Year’s Eve party at a friend’s house, the then 16-year-old David had a call from the friend’s father to say she was seriously unwell with meningitis. She died the next day.
‘At the funeral her dad said he didn’t want people to say her death at 16 was a waste, because she had done so much with her life. And he told us, basically: “You’re still here: make the most of it.” We didn’t discuss it at the time, but it motivated every single one of us. It definitely put the wind in my sails.’
Dr Baglow, who is deputy chair of the BMA south-east coast regional council, has made some important choices to affirm life: he works less than full time, for example, and always makes time for exercise. But he also feels strongly that we as a society should be more open and matter-of-fact about death and preparing to die.
He’s fascinated by the idea that the pattern on fishermen’s jumpers may have helped identify them if they drowned and washed up elsewhere – a recognition of death woven into life.
Dr Baglow questions the way death is used as a fixed point in shared decision-making. ‘Medical professionals may say things like, “If you don’t have this operation, you’ll probably be dead in six months.” But we don’t often discuss quality of life, which, in my opinion, is much more important than the length of time you have left.
‘We should be talking about independence, self-respect and dignity in death and having these conversations much earlier, rather than risk freaking people out by waiting till it affects them directly.’
He insists his attitude to death is personal and recognises that not everyone is so relaxed. He tries harder now to relate to patients, gives them more time and genuine conversation, recognising their feelings of isolation.
‘A patient the other day was shaking with anxiety and I gave him a little fist bump. I said, “There’s nothing I can say to make you feel better, but I promise I’ll treat you the way I’d want to be treated.” It’s about giving them connection, making them feel they’re not alone.’ Above all, he’s learnt gratitude.
‘When I was discharged from ICU and went on the trauma ward, I really liked watching the seagulls outside the window. It was a constant I found consoling.
‘Later, when I was working in that hospital, I went to see a patient who was in that same bed and asked if they liked the seagulls. Then I told them I’d been in that bed once. And they opened up, as if in a confessionary, and said, “I really like them too!” ‘Whenever I walked into that hospital, I’d look up at the window and think, “I’m so lucky”.’
The wounded healer
He’s known for his life-affirming tweets, his beaming smile and his raw honesty about all that’s led him to this point. Psychiatry registrar Ahmed Hankir makes no secret of the fact that his battle to regain his own mental health took him close to death.
Today he goes by the moniker ‘The Wounded Healer’ in his award-winning advocacy to tackle stigma around mental health – a phrase borrowed from Jung. He talks openly about parts of his life which were dark and difficult, because he wants it to help others. And because he feels it helps him too.
‘A lot of us feel forced to sanitise our stories but that doesn’t do justice to our reality,’ says Dr Hankir. ‘I’m proud of overcoming the obstacles and surviving and, dare I say, thriving. ‘You’ve heard: “Physician, heal thyself.” But what about, “Physician, reveal thyself?” By revealing, we can heal not only others, but ourselves.’
It was Dr Hankir’s determination to become a doctor that helped him overcome huge disadvantages and setbacks over years. He describes his current post at South London and Maudsley NHS Foundation Trust as his ‘dream job’. But it was that same ambition that often made his journey so challenging.
An outsider
The backdrop to much of his childhood was conflict. His parents moved to Northern Ireland in the early 1980s, to escape the fighting in their native Lebanon; Dr Hankir and his twin were born in Belfast.
‘My mother always said that at least in Belfast you’d get advance notice there would be an explosion: we didn’t have that courtesy in Lebanon.’
When Dr Hankir was 12, the family returned to Lebanon, still in the grip of civil war. But it became clear the children would not thrive there. And they were ambitious. Dr Hankir’s father had won a scholarship to study medicine in Cairo, while their grandfather had sold hummus from the back of a donkey in Haifa.
In 2000, Dr Hankir and his twin moved back to the UK. Britain was not a safe haven. At 17, he witnessed a man being kicked to death outside the kebab van where he worked in Malvern Hills. And he was often met with racism and Islamophobia, another strand of his campaign work today.
‘I was very outgoing, and I didn’t understand why when I would say, “Good morning,” people wouldn’t reciprocate. I was called an ajnabi [‘foreigner’ in Arabic] in Lebanon and a “Paki” in England. I always felt like an outsider.’
Dr Hankir had to support himself financially, through both sixth-form college and university. He was working up to 60 hours a week, cleaning, stacking shelves, anything to make ends meet.
Traumatic flashbacks
Despite all this, he won straight As and a place at medical school. He loved his studies but found it hard to integrate. He was surrounded by privilege while working 16-hour shifts in a fast-food outlet.
Then, in 2006, in his third year, ‘multiple factors’ conspired to push him to the brink. Images on TV of the conflict erupting in his hometown in Lebanon triggered severe distress. His behaviour changed and he fell out with his flatmates.
‘I must have had some kind of unconscious attachment towards them because they were like family to me, but I wasn’t family to them.’ He also, he alleges, suffered psychological abuse from a staff member he considered a ‘mentor and father figure’.
‘I confided in someone, he manipulated me, he deceived me. But he was never held accountable. I was a BAME medical student, a Muslim, and I have this mental health condition. The triple whammy. Who’s going to believe me?’
Then, a misunderstanding with his medical school about which cycle he was sitting exams for – ‘I showed up for the wrong cycle’ – meant he ‘was forced to interrupt’ his studies. Having fought so hard to get into medical school, this was devastating. Without a grant, he was homeless, until he found a room in a derelict house in Moss Side. He woke up one morning to find his Azeri housemate had died of a drug overdose. He recalls scouring the streets for coins so he could buy out-of-date bread.
‘I was really unwell and felt suicidal,’ he says. ‘I was getting these traumatic flashbacks: I would scream and shout in the night. It was like this tempestuous howling storm in my head, and it just wouldn’t stop.’
Stay grateful
It took months before Dr Hankir was well enough to return to med school; he had to repeat two years, adding to his financial difficulties.
He often went to bed on an empty stomach. But it took years to fully regain his mental health. In his powerful presentations and lectures addressing mental health-related stigma that have won him international acclaim today, he often uses drama: theatre has played a strong role in his recovery and is an integral part of his resilience, along with cycling and running.
He regularly advocates spending time in nature and keeping a gratitude diary. His strong faith has also been central to his recovery and his resilience. ‘As a practising Muslim, I’m constantly reminded of the fragility of life. Life is so short but it’s precious.’ He has his detractors and doubters. Some on social media have accused him of ‘toxic positivity’.
'I’m constantly reminded of the fragility of life. Life is so short but it’s precious'
Dr Hankir
Others, including fellow psychiatrists, have alleged ‘fabrication’. But he’s also won several awards including, last year, a WHO Director-General Award for Global Health and The Sun’s Caroline Flack Mental Health Hero Award. It’s been a journey – and he’s still on it.
‘People might only get a snapshot of me because now life is beautiful. I’m extremely blessed and I’m grateful. But this didn’t come easy: I had to work bloody hard. But as they say in The Shawshank Redemption, “I’d rather be busy living than busy dying.” Do we want to wallow in self-pity?’
Though his past is still present, he’s determined to face forward and help others do the same.
‘In Lebanon last [month], I saw a young child begging for anti-epileptic drugs for his sister. ‘Oh, my goodness. Let’s be grateful, not bitter. Let’s learn and share and grow and be positive. There are so many reasons to stay alive and to choose life.’